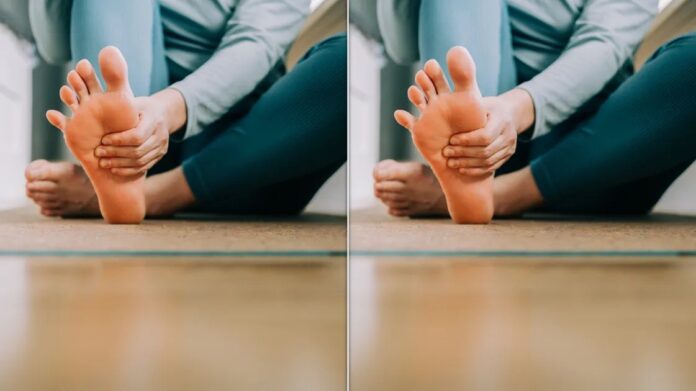
Most people walk around without giving a second thought to the structure of their feet—until pain strikes. While the foot’s arch is designed to support body alignment, absorb shock, and navigate uneven terrain, roughly 25% of adults have flat feet. This condition, medically known as pes planus, means the sole of the foot touches the ground entirely when standing.
However, having flat feet is not inherently a disease. In fact, it is often a normal variation. The critical distinction lies in whether the condition is causing symptoms. Here is what you need to know about identifying problems, understanding the mechanics, and deciding on treatment.
The Reality: Most Flat Feet Are Asymptomatic
It is important to understand that flat feet are common and often harmless. Dr. Nicole Nicolosi, a foot and ankle surgeon at the Cleveland Clinic, notes that infants are born with flat feet, and arches typically develop between ages 7 and 10.
In adulthood, genetics, injuries, or conditions like rheumatoid arthritis can lead to flat feet. Yet, statistics suggest that only about 1 in 10 adults with flat feet experience symptoms severe enough to require treatment.
“You can have a flat foot and live a long and happy life without any issues,” explains Dr. Nicolosi.
If you have flat feet but no pain, you generally do not need special inserts, medical interventions, or lifestyle changes. The absence of pain is the primary indicator that your body is handling the structure effectively.
Why Pain Occurs: The Mechanics of Compensation
When flat feet do cause issues, it is rarely because the lack of an arch hurts directly. Instead, pain arises from compensation. The body subconsciously shifts its weight to maintain balance, altering how forces are distributed across the skeletal system.
Dr. Amiethab Aiyer, division chief of foot and ankle surgery at Johns Hopkins, describes the foot as a “tripod.” In a flat-footed individual, this tripod is compromised, causing weight to shift toward the outside of the foot. This mechanical shift can trigger a cascade of problems:
- Localized Foot Pain: Pressure shifts can cause pain on the outer side of the foot, just in front of the ankle, or along the back of the ankle.
- Plantar Fasciitis: The strain on the plantar fascia (the band of tissue connecting the heel bone to the toes) can lead to inflammation and discomfort.
- General Fatigue: Many individuals report a dull ache or quick fatigue in their feet after standing or walking.
The Ripple Effect: Beyond the Feet
The impact of flat feet often extends far beyond the ankles. Because the foot is the foundation of the body’s kinetic chain, altered mechanics can affect joints further up the leg.
Dr. Nicolosi warns that changes in gait (walking pattern) can increase wear and tear on the knees and hips, making individuals with flat feet more prone to developing arthritis in these areas. “Everywhere down the line, everything’s connected,” she notes. This systemic connection highlights why addressing foot mechanics is often about protecting the entire lower body, not just the feet.
Tendonitis: A Common Complication
Another frequent issue for those with flat feet is posterior tibial tendonitis. The posterior tibial tendon is the primary structure responsible for supporting the arch. In flat feet, this tendon is often stretched or deficient, making it susceptible to inflammation.
While this may not always lead to severe disability, it can cause:
* Periodic inflammation
* Tenderness along the inner ankle
* Dull, persistent pain
When to See a Doctor
Not all flat feet require intervention, but certain signs indicate that medical advice is necessary. You should consult a healthcare provider if:
- Pain interferes with daily life: If you experience pain during regular activities, limping, or notice a change in your walking pattern.
- Sudden onset: If you never had flat feet but suddenly do, particularly after an injury. This could indicate damage to the structures supporting the arch, such as a tendon tear.
- Progressive symptoms: If pain or discomfort is worsening over time.
Treatment Options and Prevention
If symptoms are present, treatment focuses on restoring alignment and reducing strain. Options typically include:
- Orthotics: Custom or over-the-counter inserts with arch support are a “mainstay” of treatment. They help alleviate pressure on the posterior tibial tendon and correct alignment, potentially preventing arthritis and gait abnormalities.
- Physical Therapy: Exercises to strengthen foot and ankle muscles can improve stability.
- Surgery: In rare, severe cases where conservative treatments fail, surgery may be recommended to reconstruct the arch.
For those without symptoms, the best preventive measure is simple: wear supportive shoes. Proper footwear helps maintain foot health and prevents future issues, ensuring that flat feet remain a non-issue rather than a source of chronic pain.